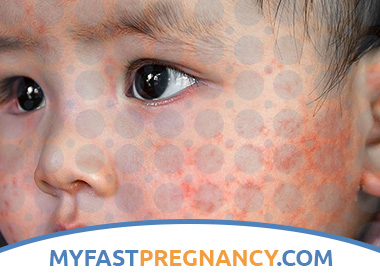
What is Atopic Dermatitis in Children?
Atopic dermatitis is the most common form of eczema. Atopic dermatitis mainly occurs in children, but may also appear in adulthood. Eczema is a chronic skin disease in which the skin turns red, itching, cracks appear, it becomes dry. Atopic dermatitis accounts for 30% of all skin diseases. The disease appears equally in both boys and girls. In recent years, doctors have noted an increase in the development of the disease. Atopic dermatitis can affect any part of the skin on the body, as a rule, the disease is localized on the arms, legs, under the knees, ankles, wrist, face, neck and upper chest.
Causes of Atopic Dermatitis in Children
Atopic dermatitis occurs in children with hereditary tendencies, hypersensitivity, hay fever, asthma, chronic urticaria and other types of eczema. Atopic dermatitis in other words inherited dermatitis. Atopic dermatitis may worsen under the influence of external environmental factors such as pollen, hair and epidermis of domestic animals, and internal factors such as hormones and stress. Approximately 80% of cases begin in children under the age of 5 years. A significant number of cases develop during the first year of life.
60% of children with atopic dermatitis have one of the parents with the same disease.
Atopic dermatitis can cause the use of antibiotics in children. Studies show that the use of antibiotics in early childhood may increase the risk of developing eczema by 40%.
Pathogenesis during Atopic Dermatitis in Children
Studying the disease, scientists have discovered a gene that causes dry, scaly skin and predisposes people to eczema. Defects in the filaggrin gene are associated with a significant increase in the risk of developing allergic diseases such as eczema, rhinitis, asthma, etc.
As a rule, the lipid (epidermal) skin barrier decreases in people with atopic dermatitis. Lipid barrier function – to prevent moisture loss. If the barrier decreases the skin loses fluid faster, and as a result it becomes dry.
Symptoms of Atopic Dermatitis in Children
Atopic dermatitis is a long-term, chronic condition. With an exacerbation of the disease, the symptoms worsen and the patient needs more intensive treatment.
Atopic dermatitis begins with unpleasant itching. The more the child scratches the skin, the more it itches, which can lead to bleeding. Let’s note the general symptoms of atopic dermatitis: redness, inflammation and dryness of the skin, itching (worse at night), cracks, moist discharge in the area of scratches on the skin (scratches can lead to thickening of the skin), blisters, brownish-gray skin color, bumps
Some patients have eczema eruptions around the eyes, including on the eyelids. Scratching the eye area can eventually lead to noticeable loss of eyebrows and eyelashes. Babies usually have facial rashes.
With an exacerbation in patients, there is: increased itching (itching and scratching make the skin redder and more sensitive), there is a burning sensation in the affected areas, the skin becomes more scaly and dry, the bumps are more pronounced, the affected areas are susceptible to infection with bacteria. The aggravation lasts from a day or two to several weeks.
People with mild atopic dermatitis usually have small patches of dry skin that can sometimes itch. With severe symptoms, many itchy areas ooze. Children with atopic dermatitis have severe sleep disturbances that affect concentration at school during class.
Some factors can aggravate the symptoms of the disease, they include: prolonged hot showers or baths, mental stress, hormones, sweating, sudden changes in temperature, dry air, some types of clothing materials (wool), dust, sand, some household products. There are also environmental factors that affect the deterioration of clinical signs: allergens (pollen, dust mites, animal dander) – cause a disorder of the body’s immune system, an allergic reaction, hard water. These three allergens are also major contributors to asthma and hay fever.
Diagnosis of Atopic Dermatitis in Children
The diagnosis of the disease is made on the basis of symptoms and minor laboratory tests. During the examination, the patient and parents are asked typical questions about the presence of eczema among close relatives, about a tendency to allergic diseases (asthma, hay fever, etc.).
The doctor can assess the condition of the patient’s skin according to a number of diagnostic criteria in order to confirm the diagnosis of atopic dermatitis. Criteria may include:
- The duration of the itching period (the last year is taken into account).
- Itching and irritation of the skin in areas such as elbows, under the knees, ankles, neck, eyes.
- Having asthma and hay fever now or in the past.
- The presence of dry skin (take into account the last year, the period of the appearance of dryness).
- Scaly on joints, wrists, knees, or elbows.
As a rule, the above criteria are sufficient for a doctor to diagnose.
When diagnosing, it is important for a doctor to find out the factors that influenced the onset of the disease and the development of symptoms. The doctor will ask the patient or parents about the lifestyle, the foods they eat, and the home environment.
The doctor will definitely carry out differential diagnostics in order to exclude other skin diseases such as contact dermatitis, prickly heat, seborrheic dermatitis and psoriasis.
The patient will definitely be assigned allergy tests to establish a potential allergen.
Treatment of Atopic Dermatitis in Children
There is currently no cure that will get rid of the disease permanently. However, there are many treatments available that are aimed at relieving symptoms and improving quality of life. Treatment is:
Medication therapy:
- Corticosteroids reduce inflammation, irritation, and itching. If the person’s skin is very red and inflamed, the doctor may prescribe topical corticosteroids. Parents should not be intimidated by these funds, they are safe and effective.
- Antihistamines – Reduces allergic reactions. The course of treatment with antihistamines is approximately 14 days. Conversely, some sedatives can be used on a long-term basis. While taking sedative antihistamines, patients may become drowsy. They will help relieve itching, but they won’t get rid of the infection. Antihistamines include diphenhydramine hydrochloride or hydroxyzine hydrochloride.
- Antibacterial agents are prescribed for severe symptoms, infection. The antibiotic flucloxacillin is most often prescribed, the course of treatment is 7 days. The doctor may prescribe alternative antibiotics such as erythromycin or claritomycin.
- Antiseptic drugs are applied directly to the affected area of the skin. These drugs include: chlorhexidine, triclosan, etc.
- Immunomodulators are used twice a day in children over the age of two. Their action is aimed at blocking the exacerbation of the disease. They are used at the first sign of itching or rash.
Light therapy (phototherapy) involves the use of natural or artificial light. Patients should be exposed to natural sunlight frequently. Other forms of phototherapy include the use of artificial ultraviolet light. Light therapy is very effective. Exposure to sunlight has many beneficial effects, but there are risks nonetheless: premature skin aging and a high incidence of skin cancer.
Ancillary treatments. They are very popular among patients with atopic dermatitis. These include aromatherapy, massage, herbal baths (peony root, mint, etc.), homeopathy and some herbal remedies, acupuncture.
Emollients: lotions and ointments – soften and smooth the skin, keep it firm and moist. Emollients are very important during the treatment of atopic dermatitis, which helps prevent cracking and irritation of the skin. Creams and lotions are usually used for reddened, inflamed areas, while ointments are used for dry areas that are not inflamed. These remedies are often used to prevent worsening of outbreaks. The use of funds on the affected areas significantly reduces the severity of the disease.
The use of special anti-allergenic agents (soap, shampoo, shower gel).
In severe cases of atopic dermatitis, patients may experience complications:
- Development of infection. If your skin is dry, cracked, or scratched, the risk of bacteria getting in increases, for example, Staphylococcus aureus is more common. Staphylococcus aureus infection worsens the symptoms of atopic dermatitis, causing increased redness, excessive fluid discharge, and crusting on the skin.
- Mental stress. Living with atopic dermatitis can have a psychological impact on the sufferer, especially if the illness began at an early age. Children with atopic dermatitis have more behavioral problems in school than their peers. Parents sometimes note that a child with atopic dermatitis is much more stubborn than other children.
- Stress. Children develop stress due to being teased and bullied about their skin condition. Children with eczema are insecure. The family must support the child in helping to overcome this problem. If self-confidence is seriously compromised, parents should seek help from a psychologist.
- Most children with atopic dermatitis have trouble sleeping. Lack of sleep can affect a person’s physical and mental health.
Prevention of Atopic Dermatitis in Children
The disease can be controlled by avoiding scratches and provoking factors, by diet, taking additional medications (corticosteroids, antihistamines, antibiotics (in case of infection), taking courses of light therapy.
About 10% of children with atopic dermatitis suffer from food allergens found in cow’s milk, eggs, nuts, soy, and wheat, so they should be eliminated from the diet. Therefore, it is important, together with a nutritionist, to develop an individual diet, excluding food allergens. The doctor selects an alternative substitute for them.
Scratching increases the risk of infection. Children find it difficult to resist scratching the affected areas. Children are often unable to control their desire. Therefore, it is important for parents to keep their nails short and clean. Scratches can be worn for babies.
For preventive purposes, it is necessary to avoid provoking factors that affect the exacerbation of the disease. Parents should constantly remind their children of allergens.
Clothes made of synthetic fibers are contraindicated for children with atopic dermatitis. Parents should choose natural materials such as cotton.
To avoid dry skin, it is shown to take a daily warm bath with mild special hypoallergenic agents that retain skin moisture.