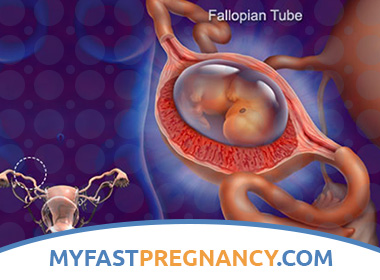
What is Ectopic Pregnancy?
An ectopic pregnancy is an abnormal pregnancy that poses a serious threat to a woman’s life. Instead of developing, as expected, in the uterus, a fertilized egg develops outside it. Most often (in 99% of cases) it is fixed in the fallopian tube, but may be in the ovaries and in the abdominal cavity.
Causes of Ectopic Pregnancy
The risk of ectopic pregnancy increases with age and is highest in women 35-44 years old. Particularly attentive to yourself should be women suffering from chronic inflammatory diseases caused by chlamydial infection, mycoplasma or ureaplasma, as well as those who have been treated for tubal and hormonal infertility. In addition, the risk group includes women with endometriosis, congenital anomalies of the uterus and fallopian tubes, miscarriage. The use of an intrauterine device as a contraception can also provoke an ectopic pregnancy.
An ectopic pregnancy is a dangerous condition when an egg fertilized in the fallopian tube cannot reach the uterus in time.
The main cause of ectopic pregnancy is blockage of the fallopian tube or violation of its contractions.
This can happen when:
- inflammatory processes in the genitals (ovaries and tubes) – for example, after an abortion;
- congenital underdevelopment of fallopian tubes;
- hormonal disorders;
- tumors of the internal genital organs.
Pathogenesis during Ectopic Pregnancy
If the fertilized egg does not fall into the uterus, it is attached in the place where it is, for example, to the wall of the fallopian tube, and there begins to grow. However, the tube is not intended for the development of the fetus: its thickness is only from 1 millimeter to 1.5 centimeters, and the thin and delicate wall is not capable of stretching, like a uterus. Therefore, at some point the place for the development of the fetus becomes insufficient.
At about the 4th-6th week of ectopic pregnancy, the villi of the outer shell of the embryo germinate the wall of the fallopian tube – it breaks and bleeding into the abdominal cavity occurs. This causes a sharp cramping pain in the lower abdomen, nausea, dizziness, and often loss of consciousness. If a large vessel is damaged, a woman may lose a large amount of blood, which is deadly.
Sometimes it is not the tube that breaks, but the wall of the ovum, which is then expelled into the abdominal cavity through the end of the fallopian tube. This case is called tube abortion. It is also accompanied by severe pain in the lower abdomen, weakness and dizziness, but these symptoms develop more slowly than when a pipe breaks. After some time, the pain subsides, and the woman gets the impression that she is fine. However, continued bleeding into the abdominal cavity can lead to the same grave consequences as with a ruptured ectopic pregnancy tube.
Symptoms of Ectopic Pregnancy
Clinic and diagnosis of tubal abortion. The clinical picture of tubal abortion develops for a long time and is determined by doubtful (nausea, vomiting, changes in olfactory and taste sensations, drowsiness, weakness) and likely (engorgement of the mammary glands, delayed menstruation) signs of pregnancy, on the one hand, and symptoms of tubal pregnancy interruption, on the other. When menstruation is delayed, most often at 2–3 weeks, patients note recurrent bouts of cramping abdominal pain radiating to the rectum, poor dark blood discharge from the genital tract. Blood discharge due to rejection of decidually modified uterine mucosa due to abortion. Sometimes a woman does not notice a delay in menstruation, but on the days of menstruation, poor blood discharge appears from the genital tract. Pain is associated with a contraction of the fallopian tube, as a result of which the fertilized egg partially or completely exfoliates from its walls, blood is poured from the fallopian tube into the abdominal cavity. The severity of complaints and the general condition depend on the amount of blood poured into the abdominal cavity and the speed of blood loss.
With a small intra-abdominal blood loss, the general condition of the patients does not suffer, the pain can be aching, and slight. Sometimes the symptoms are so scarce that it is rather difficult to identify the disease.
Upon admission into the abdominal cavity of more than 500 ml of blood, severe pain appears with irradiation to the right hypochondrium, interscapular region and right clavicle (phrenicus symptom). Often there is weakness, dizziness, fainting, vomiting.
Blood tests can show a decrease in hemoglobin level, a picture of hypochromic anemia, a shift in the leukocyte formula to the left, and an increase in the ESR.
Diagnostic help additional research methods. For recognition of ectopic pregnancy ultrasound scan of the pelvic organs is widely used. The results of echographic research should be considered only in conjunction with data from other diagnostic methods. The absolute ultrasound sign of ectopic pregnancy is the detection of the ovum with the embryo near the body of the uterus.
If an ectopic pregnancy is suspected, it is recommended to determine the level of chorionic gonadotropin (CG) in the blood over time. The information content of the study of CG is 96.7%. With ectopic pregnancy, the titre of chronic hepatitis increases more slowly than with uterine, and does not correspond to the duration of pregnancy. However, even the definition in the dynamics of the titre of CG does not always allow to reliably distinguish ectopic pregnancy from complicated uterine. Interruption of any pregnancy leads to the death of the chorion, the cessation of CG production, therefore a negative pregnancy test does not exclude ectopic pregnancy.
Until now, in clinical practice, puncture of the abdominal cavity through the posterior fornix of the vagina has been used to diagnose ectopic pregnancy, although this method has lost its significance if laparoscopy is possible. In an ectopic pregnancy, dark, uncontrolled blood is obtained with chorionic villi that float up when the item is placed in a vessel with water. The results of abdominal puncture may be either false-positive if the needle enters the parametrium or uterus vessel, or false-negative if there is a defect in the needle, a small amount of blood in the abdominal cavity, blood clots or a pronounced adhesive process in the uterine appendages. Blood during puncture of the zagochente space can also be detected during ovarian apoplexy, rupture of parenchymal organs, menstrual blood reflux, after curettage of the uterine mucosa.
If an ectopic pregnancy is suspected, diagnostic curettage of the uterine mucosa with a histological examination of the endometrium is used for differential diagnosis of dysfunctional uterine bleeding or incomplete spontaneous abortion.
The most accurate method for the diagnosis of ectopic pregnancy is laparoscopy, which makes it possible to visually assess the condition of the pelvic organs, including the fallopian tubes.
Clinic and pipe rupture diagnostics. Symptoms of rupture of the fallopian tube is quite bright, due to acute intra-abdominal bleeding and does not create any diagnostic problems. Abdominal pain appears with complete well-being (often a sharp pain occurs on the side of the “pregnant” tube), radiates to the rectum, the right collarbone (phrenicus symptom), often tenesmus and loose stools. Observed “severe weakness, then loss of consciousness, with a large intra-abdominal blood loss – hemorrhagic shock. Patients are apathetic, inhibited, pallor of the skin and visible mucous membranes, cold sweat, shortness of breath are noted. Pulse frequent, weak filling and tension, blood pressure decreases. The abdomen is swollen, tense in the lower parts, on palpation there is a sharp pain and symptoms of peritoneal irritation, dullness of percussion sound in sloping areas of the abdomen, the boundary of which is mixed with the change of body position. Gynecological examination reveals cyanosis of the mucous membrane of the vagina, and blood discharge from the cervical canal is often absent. A bimanual examination reveals an excessive mobility of the enlarged, softened uterus (a symptom of a “floating uterus”), sharp pain during cervical dislocations, an overhang and marked soreness of the posterior vaginal fornix (“Douglas cry”). Due to the bright clinical picture of uterine rupture, there is usually no need to use additional research methods.
The clinical picture of the interruption of rare forms of ectopic pregnancy (ovarian, abdominal, or rudimentary horn pregnancy) differs little from the clinical picture when tubal pregnancy is interrupted and is characterized by large intra-abdominal blood loss. The final diagnosis is made during surgery.
Interruption of an ectopic pregnancy is a serious danger to the health of a woman, therefore, timely diagnosis of a progressive tubal pregnancy is very important.
Clinic and diagnosis of progressive tubal pregnancy. Prevention of tubal abortion and rupture of the pipe to a large extent lies in the timely diagnosis and treatment of progressive tubal pregnancy. Progressive tubal pregnancy does not cause an acute abdomen clinic. In fact, the clinic of progressive tubal pregnancy is similar to that for uterine pregnancy of small periods.
Patients have questionable and probable signs of pregnancy (delayed menstruation, engorgement of the mammary glands, changes in taste, appetite, smell, etc.).
In the case of a two-handed vaginal-abdominal examination, there is a discrepancy between the size of the uterus and the gestational age, sometimes the spindle-shaped formation of a soft or elastic consistency in the area of the uterine appendages, painful on palpation, is determined. However, with a short period of pregnancy, the increase in the fallopian tube is insignificant, so it cannot be detected. Signs of uterine pregnancy most often not detected.
For the diagnosis of progressive tubal pregnancy, the additional methods of research described earlier — ultrasound scanning, determination of CG level in the blood, and laparoscopy are of particular importance.
Diagnosis of Ectopic Pregnancy
In order not to risk your health, on the 4-7th day after the delay of menstruation you should contact a gynecologist. Modern diagnostic methods, including ultrasound, allow us to establish pregnancy in the early stages and to determine whether it is ectopic. Ultrasound examination is especially recommended for women in whom delayed menstruation is accompanied by bloody discharge.
At the slightest suspicion of an ectopic pregnancy, the doctor suggests that the woman should go to the hospital. Do not refuse: only in a specialized institution equipped with modern equipment, it is possible to conduct the necessary research and determine where the germ is implanted – in the uterus or outside it.
Treatment of Ectopic Pregnancy
Treatment of ectopic pregnancy is to stop intra-abdominal bleeding by surgery, restoration of impaired hemodynamic parameters and, if necessary, rehabilitation of reproductive function.
When establishing both interrupted and progressive ectopic pregnancy, an emergency operation is performed. Indication for immediate laparotomy is hemorrhagic shock.
Most often during tubal pregnancy, a tube is removed (tubectomy). However, in some cases, under appropriate conditions, organ-preserving (conservative-plastic) operations are performed to preserve reproductive function: squeezing the “milking” fetal egg (when localized in the fimbrial section), tubotomy is the incision of the fallopian tube at the location of the fetal egg and its subsequent removal ( with small sizes of the ovum), resection of the fallopian tube segment. Indications for tubectomy are repeated pregnancies in the fallopian tube, previously subjected to conservative intervention, cicatricial changes in the fallopian tube, unwillingness to have a pregnancy in the future, rupture of the fallopian tube, the diameter of the ovum more than 3.0 cm.
It should be noted that after organ-sparing operations, including with a single fallopian tube, the risk of re-ectopic pregnancy increases. However, the frequency of uterine pregnancy after conservative plastic surgery is higher than after in vitro fertilization.
When ovarian ectopy of the ovum is ovarian resection within healthy tissue. Pregnancy in the rudimentary horn of the uterus requires removal of the rudimentary horn. Surgical treatment of abdominal pregnancy is often associated with great technical difficulties and, if possible, consists in excision of the fetal stem with careful hemostasis.
Patients who have undergone surgery in connection with an ectopic pregnancy, need to further restore menstrual and generative functions. After the operation, almost half of the women have neuroendocrine and vegetovascular disorders, and later infertility occurs, and the risk of repeated ectopic pregnancy increases. Rehabilitation measures consist in prescribing antibacterial therapy for the prevention of the inflammatory process, physiotherapeutic procedures that reduce the possibility of the formation of adhesions in the pelvis, iron preparations, and vitamins.
Important importance after surgery for ectopic pregnancy is given to contraception, preferably combined oral contraceptives. The duration of pregnancy should not be less than 6 months.
Conservative treatment of ectopic pregnancy. In recent years, work has emerged on the conservative treatment of progressive tubal pregnancy. To date, there is no consensus on both drugs for the conservative treatment of ectopic pregnancy, and their doses, duration of administration and methods of administration. Local injections of methotrexate, controlled by transvaginal ultrasound monitoring, are used.
However, this method is quite often accompanied by complications (bleeding from the mesosalpinx) and can end with a laparotomy. In recent years, there has been a tendency to use endoscopic control.
The use of drugs for the treatment of ectopic pregnancy under the control of laparoscopy is possible when the size of the ovum is no more than 2-3 cm. With the laparoscopic method of local administration of cytostatic, unlike ultrasound, it is possible to visually assess the condition of the fallopian tube, to determine the presence or absence of ectopic pregnancy. Laparoscopy allows the most accurate determination of the safe puncture point of the fallopian tube, as well as, if necessary, to ensure hemostatic manipulations. Dynamic laparoscopy provides everyday monitoring of the state of the fallopian tube after the introduction of drugs.
Most authors are unanimous in the opinion that conservative methods of treatment of ectopic pregnancy with the use of drugs may be promising, but many of the provisions require further study. In modern practical gynecology, the surgical method for the treatment of ectopic pregnancy remains more studied and priority.
Prevention of Ectopic Pregnancy
First of all – time to treat inflammatory processes in the pelvis. Before the planned pregnancy, it is necessary to make a comprehensive examination for the presence of chlamydia, mycoplasma, ureaplasma and other pathogenic microbes in order to get rid of them as soon as possible. This examination along with you must pass a husband (or a permanent sexual partner).
Do I need to once again mention the modern methods of contraception? Abortion is still the main culprit in ectopic pregnancy. Therefore, the main focus of modern medicine remains the promotion of reliable and safe methods of family planning, and in the event of an unwanted pregnancy, the operation should be performed at the optimum time (during the first 8 weeks of pregnancy), necessarily in a medical institution by a highly qualified doctor with adequate anesthesia and with the subsequent prescription of post-abortion rehabilitation.
The choice, if possible, should fall on the non-surgical interruption of pregnancy with the drug Mifegin. Of course, they are more expensive, but in this situation, saving on health is hardly appropriate. Of the classical methods, the preferred “mini-abortion”, which has a minimal incidence of side effects due to minimal trauma to the uterus and reduce the time of surgery.
After surgery for ectopic pregnancy is very important rehabilitation, aimed at preparing for the next pregnancy. Usually it takes place under the supervision of a gynecologist, in several stages. Experts believe that the best time for a new pregnancy is six months – a year after a tube operation.